clinical genetics
Bringing Genetic Results to Your Doctor: A Prep Guide
A 15-minute appointment can't absorb a 600,000-row raw DNA file. Here is how to prep a clean, structured genetic handoff your clinician can actually act on in the room.
Sebastian Thorp · May 1, 2026 · 6 min read

In short
A typical primary-care appointment is 15 minutes. Your raw genotype file is hundreds of thousands of rows long. The gap between those two facts is where most "I want to discuss my DNA results with my doctor" conversations fall apart. This guide is a four-step playbook for prepping a clinician handoff that actually works: get a structured report, identify the two or three findings worth discussing, prepare specific questions, and bring the printed PDF. It also covers what not to do — anxiety-spiraling, self-diagnosing, demanding tests your insurance won't cover.
The structural problem
Clinicians don't refuse to look at genetic data because they don't care. They refuse — or change the subject quickly — because the format makes it impossible to act on inside an appointment slot. You can't usefully review 600,000 variant calls between two patients in a packed schedule. You also can't act on a list of findings without knowing which two or three actually warrant discussion versus background noise.
The fix is on the patient side. Bring something a clinician can read in 30 seconds, focused on a small number of decisions, with primary-source citations they can verify if they want to.
Step 1 — Get a structured report
Don't bring the raw file. Don't bring a 50-page printout from Promethease. Bring a structured PDF that organizes findings by clinical relevance — typically:
- An executive summary at the top (3–5 lines)
- Highest-priority findings with citations
- Drug-gene interactions for medications you're on or considering
- Carrier status notes if relevant to your situation
- A monitoring schedule (what to recheck and when)
A purpose-built tool produces this format directly with primary-source citations a clinician can verify. If you're using a more raw output, spend 30 minutes summarizing it into a one-page document yourself before the appointment. The format is more important than the breadth.
Step 2 — Identify two or three findings worth discussing
Even a well-structured report often has more findings than fit a 15-minute appointment. Pick at most three. Use these criteria, in order:
- Decision-relevance. Does this finding change something you'd otherwise do? An MTHFR finding that suggests switching from synthetic to methylated B-vitamins is decision-relevant if you're taking a B-complex. It's not, if you aren't.
- Drug-related. Pharmacogenomic interpretation is a clinical-grade workflow ordered through a prescriber — not something to derive from a consumer report. If your prescriber has ordered a clinical PGx panel, those results trump almost everything else for near-term prescribing decisions.
- Family-history convergent. A finding that aligns with your family history is worth raising even if its individual evidence is moderate, because the combined picture changes how your clinician will think about screening.
Three concrete examples:
- "My report flagged CYP2C19 *2/*2 (poor metabolizer). I'm starting sertraline next month. Does this affect dose selection?"
- "My homocysteine was 14 last month, and my MTHFR is C677T homozygous. Is methylated folate worth trying before we increase the SSRI?"
- "Both my parents had early-onset cardiovascular disease, and my report shows ADD1 and AGTR1 sodium-sensitivity variants. Should we add ambulatory BP monitoring?"
Each is one sentence, one decision, one citation in the document the clinician is holding.
Step 3 — Prepare specific questions
Open-ended questions ("what should I do about my DNA?") get vague answers. Specific questions get specific answers. The pattern that works:
[Finding] + [What I'm currently doing or considering] + [Specific question about a near-term decision].
A few templates:
- "Given [finding], should we run [specific clinical test] before [specific decision]?"
- "My report suggests [finding]. Does that change the dose / drug choice / monitoring schedule for [the medication or condition we're already discussing]?"
- "If I had [finding], would you typically refer to [specialty] or [test], or treat it as informational only?"
Write the questions out before the appointment. Bring them on paper with the report.
Step 4 — Bring the printed PDF
Email and patient portals are great for non-urgent reference. But during the appointment itself, paper sits on the desk between you. The clinician can flip to the relevant page without disrupting their workflow. Print two copies — one for them to keep, one for you to follow along.
If your clinician's practice has a portal, you can also upload the PDF in advance with a note: "I'd like to discuss the highlighted findings during our appointment Tuesday." That gives them the option to skim ahead without obligation.

What not to do
Five common mistakes that derail appointments:
- Don't anxiety-spiral on every gene. Most findings in any consumer-array report are common variants with modest effects. A finding is a starting point for discussion, not a diagnosis.
- Don't self-diagnose. "I have the Alzheimer's gene" is rarely accurate from a consumer-array report and almost never useful at an appointment. Let your clinician interpret in clinical context.
- Don't demand tests your evidence doesn't justify. A consumer-array finding rarely justifies an expensive specialist referral on its own. It can support a referral your clinician was already considering.
- Don't skip the medication list. PGx findings are uninterpretable without knowing what you're actually taking. Bring an updated medication and supplement list.
- Don't expect your primary care doctor to be a geneticist. They aren't, and they won't pretend to be. For complex findings — BRCA-adjacent variants, cardiomyopathy genes, cancer predisposition panels — ask for a referral to a genetic counselor.
When to skip the GP and go straight to a counselor
For three categories of finding, a genetic counselor is the right starting point, not your primary care doctor:
- Cancer predisposition (BRCA1/2, Lynch syndrome genes, others)
- Cardiomyopathy or arrhythmia syndrome genes
- Reproductive carrier status with family-planning implications (clinical-grade carrier panels are ordered through a healthcare provider or genetic counsellor — not derived from a consumer-array report)
Most insurance plans cover counselor referrals when there's a documented finding. The National Society of Genetic Counselors directory is a place to start.
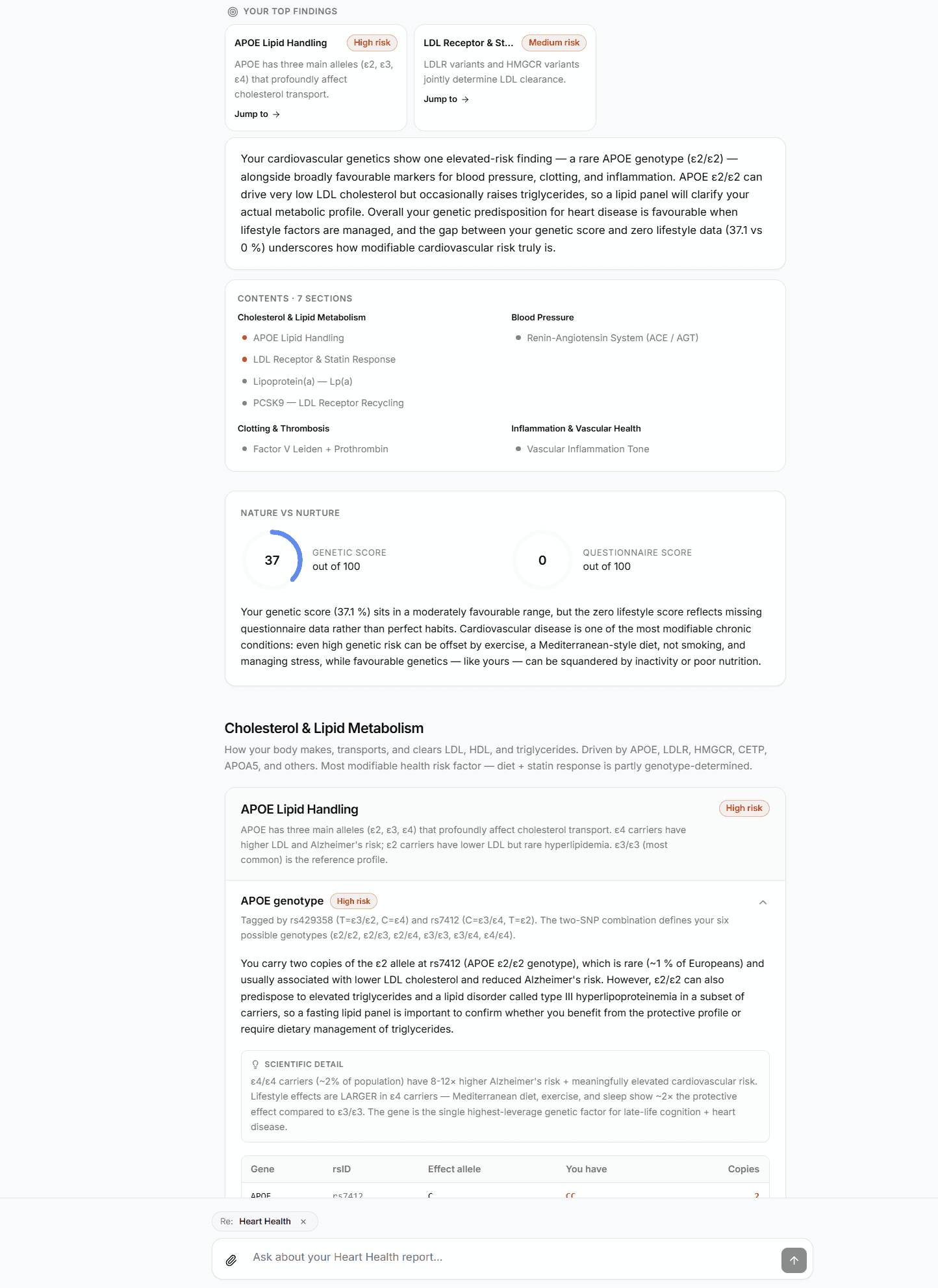
How GenoSight helps
GenoSight's report is built specifically for this use case. The PDF that gets emailed to you is structured for clinician handoff — executive summary, prioritized findings with citations, and educational genetic context to bring to the conversation. The findings-grounded chat lets you draft and refine your specific questions before the appointment. (See what's in a GenoSight report for the full structure.)
If your goal is to bring genetic data to a clinician, choose "Patient prep for clinical visit" as your goal during onboarding — the report is reformatted to lead with handoff-ready content.
Build a clinician-ready report
GenoSight produces a PDF formatted for handoff: prioritized findings, citations, monitoring schedule. Free trial.
Medical disclaimer
GenoSight provides educational information about your genetic data. It is not a medical diagnosis, treatment, or cure. Always consult your healthcare provider before making decisions based on this information. Variant interpretation evolves; recheck periodically.
Key takeaways
- A 15-minute appointment can't absorb a raw genotype file — bring a structured PDF instead, organized by clinical relevance.
- Pick at most three findings to discuss, prioritized by decision-relevance, drug-related impact, and family-history convergence.
- Specific questions get specific answers — pattern: [finding] + [what you're doing or considering] + [near-term decision].
- Bring printed copies; consider uploading to your patient portal in advance with a note about which findings to discuss.
- For cancer-predisposition, cardiomyopathy, or carrier-status findings with family-planning implications, ask for a genetic counselor referral instead of relying on primary care.